Back pain is incredibly common, and for many people it starts gradually. A sore lower back after a long day, stiffness in the morning, or discomfort after lifting something heavy can feel routine. But when…
Patients wanting to avoid artificial disc replacement complications need to understand the benefits of surgery and the type of complications, recovery challenges, and signs that something may not be healing properly afterward. Most patients recover without major issues, but no spine procedure is completely free of risk. Understanding what can happen after surgery allows patients to make more informed decisions and recognize when follow-up evaluation may be necessary.
Artificial disc replacement is often recommended for patients with degenerative disc disease, persistent nerve compression, or disc-related neck or back pain that has not improved with conservative treatment. The procedure involves removing the damaged intervertebral disc and replacing it with an artificial implant. ADR is used to treat various spinal conditions such as degenerative disc disease and spinal stenosis. The goal is to identify and remove the affected disc to restore spinal function, alleviate nerve pressure, and improve mobility.
Unlike fusion surgery, which is the traditional approach and results in permanent immobilization of the spinal segment, artificial disc replacement is designed to preserve movement at the affected spinal level rather than permanently limiting motion.
For the right patient, this approach can provide significant pain relief and improved function. At the same time, artificial disc replacement complications and recovery problems still require careful consideration before surgery. The overall complication rate for artificial disc replacement surgery is relatively low, with most patients experiencing successful outcomes post-surgery. General surgical risks include infection, bleeding, blood clots, and anesthesia reactions.
What Is Artificial Disc Replacement?
Artificial disc replacement involves removing a damaged spinal disc from the disc space and replacing it with an artificial implant designed to maintain spacing and preserve motion between the vertebrae. Cervical disc replacement surgery is commonly performed in the cervical spine and, in select cases, the lumbar spine.
The goal is to relieve pressure on nearby nerves while reducing pain caused by disc degeneration or instability. Because the procedure preserves movement, many patients consider it an alternative to spinal fusion.
Not every patient qualifies for artificial disc replacement. Factors such as spinal instability, advanced arthritis, severe degeneration, or multiple affected levels may influence whether another surgical approach is more appropriate. Complications specific to ADR surgery can arise from improper implant placement, which may lead to suboptimal functional motion and balance during weight bearing activities.
What Are the Most Common Artificial Disc Replacement Complications?
Most complications following artificial disc replacement are uncommon, but they can occur. Some develop shortly after surgery, while others appear gradually over time.
Common artificial disc replacement risks include:
- Persistent neck or back pain
- Infection around the surgical site
- Nerve irritation or continued numbness
- Implant movement or positioning issues
- Difficulty swallowing after cervical disc replacement
- Adjacent segment stress or degeneration
- Reduced mobility or stiffness
- Neck stiffness
- Limited mobility
- Dysphagia and hoarseness
- Infections at the incision site
Heterotopic ossification may limit the range of motion following artificial disc replacement surgery. Dural tears occur in approximately 0.77% of artificial disc replacement surgeries. Infections can occur at the incision site and may require antibiotics or further surgical intervention. Nerve damage can result from nerve root compression or irritation, leading to symptoms such as numbness, tingling, or weakness. Adjacent segment disease is a potential long-term complication, though artificial disc replacement may help reduce its risk by preserving spinal motion.
Some symptoms improve naturally during recovery, especially in the early weeks after surgery. Others may indicate a deeper structural or neurological issue that requires evaluation.
Pain that continues beyond the expected recovery period deserves attention, particularly if it begins interfering with walking, sleep, work, or daily movement.
Most patients can resume light activities such as driving and light work within one to two weeks after cervical disc replacement surgery, while full recovery and the ability to engage in more vigorous activities may take 6-12 weeks.
Emergency Signs of Complications
While most patients recover well after artificial disc replacement surgery, it is crucial to recognize emergency signs that may indicate severe complications. If you experience sudden, severe pain that is different from your usual discomfort, or if you notice new numbness, tingling, or weakness in your arms or legs, seek immediate medical attention. Difficulty speaking, swallowing, or breathing after disc replacement surgery are also red flags that require urgent evaluation.
Other serious symptoms include the sudden onset of severe headaches, dizziness, or loss of coordination. These could signal rare but dangerous issues such as blood vessel damage, blood clots, or other severe complications related to the artificial disc or the surgical procedure. Even a few weeks after surgery, new or worsening symptoms should not be ignored. If you notice any of these potential complications, contact your surgeon immediately to ensure prompt assessment and treatment. Early intervention can prevent permanent damage and support a safer recovery.
Signs of Failed Cervical Disc Replacement
Failed disc replacement does not always happen suddenly. In many cases, symptoms return gradually or begin changing over time.
Signs of failed disc replacement may include:
- increasing neck or back pain after initial improvement
- pain radiating into the arms or legs (radiating pain)
- numbness, tingling, or weakness
- instability during movement
- worsening stiffness or reduced range of motion
- difficulty or pain with neck movement
- neck stiffness
- arm pain
- difficulty returning to normal activity levels
When cervical disc replacement fails, patients may notice unique symptoms such as cervicogenic headaches, dizziness, or other symptoms like facial pain. Odd sensations such as numbness, tingling, or burning may indicate nerve or spinal cord issues. Patients may experience numbness or nerve pain radiating down the arm, which can signal nerve root or spinal cord compression. Spinal cord compression can cause serious neurological symptoms and requires immediate medical attention. In cases of failed cervical disc replacement, a thorough evaluation is needed to determine the cause and whether revision surgery or alternative treatments are necessary. Patient symptoms that warrant immediate medical attention include fever, difficulty breathing, and new or worsening neurological symptoms.
Some patients also describe a shift in the quality of pain. Symptoms that once felt controlled may become sharper, more constant, or more limiting during daily activity.
Imaging often plays an important role in determining whether symptoms relate to the implant itself, ongoing nerve compression, adjacent spinal levels, or another structural issue.
Artificial Disc Replacement Recovery Problems
Recovery after artificial disc replacement varies depending on the location of surgery, the severity of the original condition, and overall spinal health before the procedure. ADR surgery aims to alleviate symptoms by reducing nerve pressure and restoring spinal function.
Mild soreness, muscle tightness, and temporary nerve irritation are common early in recovery. Symptoms may fluctuate as tissues heal and inflammation settles.
Certain recovery problems deserve closer evaluation, including:
- worsening neurological symptoms
- severe pain that does not improve
- signs of infection
- new weakness
- difficulty with balance or coordination
Nerve healing often takes longer than patients expect. Some numbness or tingling may continue for weeks or months, particularly when compression existed for a long time before surgery. Early treatment of neurological symptoms such as numbness, tingling, or weakness is crucial, as it can prevent permanent nerve damage.
Recovery also depends heavily on movement patterns and activity modification during the healing phase. Returning to strenuous activity too quickly can place unnecessary stress on the surgical area. Patients should avoid heavy lifting until cleared by their surgeon.
Significant improvement is often seen within a few months after surgery. Physical therapy is an important part of recovery, helping to restore strength, flexibility, and range of motion, and supporting a safe return to normal activities.
Minimizing the Risk of Complications
Reducing the risk of complications after artificial disc replacement surgery starts well before the procedure itself. Careful patient selection, thorough preoperative planning, and choosing the right artificial disc for your specific spinal condition are all essential steps. During disc replacement surgery, experienced surgeons use precise techniques to minimize tissue trauma and ensure proper implant placement, which supports better healing and long-term function.
After surgery, following your surgeon’s instructions is key to proper healing. Attend all scheduled follow-up appointments, take prescribed medications as directed, and watch for any signs of infection or unusual symptoms. Maintaining a healthy lifestyle—such as eating a balanced diet, staying active within your surgeon’s guidelines, and avoiding smoking—can further support your recovery and reduce the risk of complications. By working closely with your healthcare team and adhering to their recommendations, you can help ensure the best possible outcome from your artificial disc replacement.
Disc Replacement vs Fusion Complications
Patients comparing artificial disc replacement and spinal fusion often focus on recovery time and long-term mobility. Both procedures have advantages and limitations, but the complication profile differs slightly between them.
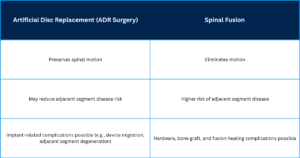
Fusion surgery involves permanently joining vertebrae, often using a bone graft to restore stability after the damaged disc is removed. This eliminates motion at the affected level, which can increase force transfer to nearby discs over time and raise the risk of adjacent segment disease. In contrast, artificial disc replacement (ADR surgery) preserves spinal motion at the treated level, which may reduce stress on adjacent spinal segments and lower the risk of adjacent segment degeneration.
Potential differences between the procedures include:
ADR surgery has its own risks, such as device migration or adjacent segment degeneration, and requires careful follow-up care and rehabilitation to ensure successful outcomes.
The best procedure depends on the patient’s anatomy, symptoms, imaging findings, and overall spinal condition. One approach is not automatically better than the other in every situation.
Long-Term Outcomes of Disc Replacement
For many patients, artificial disc replacement surgery leads to lasting pain relief and improved neck mobility, allowing a return to normal activities and a better quality of life. Most patients experience significant improvements in neck pain and function, especially when the procedure is performed by experienced surgeons and followed by appropriate rehabilitation.
However, some individuals may continue to experience persistent pain, numbness, or weakness after cervical disc replacement. In rare cases, these symptoms may indicate a failed cervical disc replacement, and revision surgery could be necessary to address the underlying problem. Long-term outcomes depend on several factors, including the severity of the original spinal condition, overall health, and adherence to postoperative care.
Discussing your unique situation and risk factors with your spine surgeon is essential to determine if artificial disc replacement is the right treatment option for you. With proper care and realistic expectations, many patients achieve better outcomes and long-term pain relief following disc replacement surgery.
When to Follow Up With a Spine Specialist
Persistent symptoms after surgery should not be ignored, especially when pain begins limiting movement or daily function again.
Follow-up evaluation may be necessary when:
- symptoms steadily worsen
- weakness develops
- mobility declines
- pain returns after initial improvement
- recovery feels significantly delayed
At Orthopedic & Laser Spine Surgery (OLSS), evaluation focuses on identifying the source of symptoms rather than assuming all postoperative pain follows a normal recovery pattern. Imaging, physical examination, and symptom progression all contribute to determining the next step.
Some patients improve with conservative management and rehabilitation. Others may require additional intervention depending on the underlying cause.
A Realistic Perspective on Artificial Disc Replacement
Artificial disc replacement can provide meaningful relief for properly selected patients, particularly when conservative treatment has failed and symptoms continue affecting daily activity. Many patients recover well and return to normal movement with reduced pain.
At the same time, understanding artificial disc replacement complications, recovery problems, and potential long-term concerns remains an important part of the decision-making process. Recognizing symptoms early and maintaining realistic expectations during recovery often improves both outcomes and patient confidence throughout the process.
If you are considering artificial disc replacement or have concerns about symptoms after spine surgery, the team at Orthopedic & Laser Spine Surgery (OLSS) can evaluate your condition and discuss treatment options based on your symptoms, imaging, and spinal health.