Sitting feels like rest, but for the lower spine, it often creates more stress than relief. Patients dealing with sciatica frequently notice that their symptoms intensify after long periods of sitting, especially during workdays, commuting,…
A herniated or slipped disc is the result of a disc moving out of place and applying pressure on nearby nerves or nerve roots. This is a very common problem because this injury often occurs during a variety of everyday events. Engaging in repetitive movements, improper lifting, or even carrying around excess abdominal weight can all result in a lumbar herniated disc.
In addition, as time goes by, we become much more susceptible to disc-related injuries. Our discs begin to break down, dry out, and tear. Furthermore, certain genetic factors may also make a person more susceptible to disc degeneration and a resulting herniated disc.
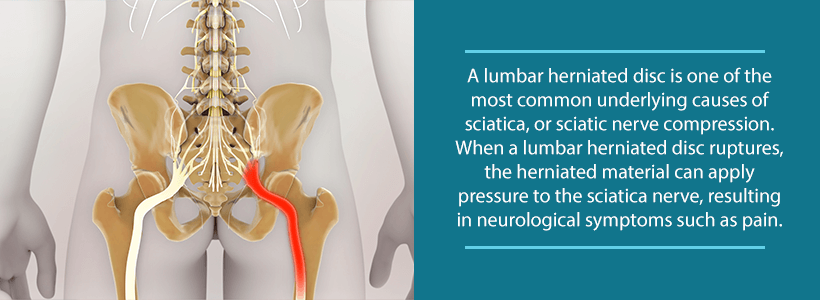
In the body, you have two sciatic nerves. These are the largest nerves in your entire body. They originate in the spine and extend all the way down the leg to the foot. You might already see where this is going. Herniated discs may put pressure on adjacent nerves, leading to neurological symptoms and pain. In the lumbar spine, the sciatic nerve just happens to be an adjacent nerve. So, when a herniated disc occurs at this point on the spine, it may lead to sciatica.
Lumbar Herniated Disc & Sciatica Symptoms
It is not uncommon for a herniated lumbar disc to put stress upon or inflame nearby nerves, leading to pain radiating along the length of the nerve. In fact, the most common cause of sciatica is a lumbar herniated disc.
These are some general characteristics of how a lumbar herniated disc may feel:
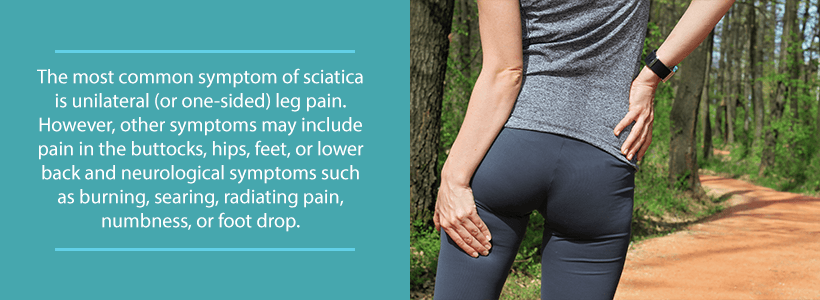
- Leg Pain: The leg pain associated with sciatica and lumbar herniated discs is much worse than the accompanying lower back pain. If the pain radiates along the sciatic nerve, then doctors call this condition sciatica.
- Variable List of Symptoms: A lot of factors determine the symptoms associated with both lumbar herniated discs and sciatica. This list includes the severity of the herniation, as well as other symptoms present in the back, buttock front/back of the thigh, calves, foot, and toes. Typically, however, the symptoms just affect one side of the body.
- Nerve Pain: Nerve pain from both conditions is very noticeable. Patients describe this kind of pain as searing, sharp, radiating, or piercing.
- Foot Drop: Foot drop is a condition that occurs when the patient has difficulty lifting the foot when walking, or perhaps when they stand on the ball of their foot. This is a neurological symptom that may occur with either condition.
- Neurological Symptoms: “Pins-and-needles” sensations, weakness, and tingling are all associated with both conditions.
- Quick Onset: Symptoms of lumbar herniated discs usually have a quick onset, but there are some cases in which symptoms develop gradually.
- Movement Pain: Sitting, standing, leaning forward, coughing, sitting for prolonged periods of time. All of these become painful with sciatica and lumbar herniated discs.
- Lower Back Pain: Lower back pain is sometimes present, but not in all cases. Aside from lower back pain, both conditions may result in stiffness, muscle spasms, and throbbing.
Rarer Symptoms of Sciatica & Lower Herniated Discs
Loss of bladder/bowel control, numbness in the saddle region, lower back pain, and weakness in the extremities are all signs of a condition known as cauda equina syndrome. This syndrome is quite rare, but if you believe you have it then you should seek medical attention immediately.
The stress and swelling of the nerves at the end of the spine may lead to paralysis and other lifelong impairments if you do not seek treatment immediately. Always, always seek out medical attention promptly if you believe you have cauda equina syndrome.
Causes & Risk Factors of Lumbar Herniated Discs with Sciatica
Lumbar herniated disc and sciatic pain may have a sudden onset, but usually, the condition comes on more gradually. Spinal discs have high water content, which helps these discs stay flexible to absorb the daily shock that the spine undergoes. Over time, these structures dry out, which leaves the disc’s tough outer shell more brittle and susceptible to cracking or tearing.
Less common causes of herniated discs include traumatic injuries, which could involve anything from a car accident to a fall. An injury may put so much pressure on the discs in the lower back that they herniate.
Here are some common risk factors for developing sciatica and lumbar herniated discs:
- Gender: Men are at twice the risk for developing lumbar herniated discs, which also increases their chance of developing sciatica that much more.
- Age: The most common age group for developing lumbar herniated discs is ages 35-50. After age 80, the condition usually does not cause symptoms.
- Physically demanding or repetitive work: Jobs that require heavy lifting or other such physical labor will put patients at a greater risk of developing lumbar herniated discs, and thereby sciatica. This is especially true for twisting actions.
- Obesity: When the spine has to support more weight, it is put under more stress. This only makes sense. Obese patients are 12 times more likely to have the same disc herniate twice. Doctors call this phenomenon recurrent disc herniation.
- Family History: People with a family history of disc herniation are much more likely to have their disc herniate than others.
- Smoking: Nicotine limits the blood flow to the discs, which exacerbates disc herniation and dampens healing. Degenerated discs are much more likely to tear and crack, leading to herniation.
Lumbar Disc Herniation & Sciatica Treatment
Most doctors will exhaust conservative options before considering surgery. Most cases of lumbar disc herniation resolve themselves within six weeks, so doctors urge patients to try more conservative options first. This does not work for everyone, however.
Nonsurgical Treatment
Here is a list of conservative options that many patients use to achieve herniated disc relief:
- Medications: Usually consist of muscle relaxants and NSAIDs. This is also great for sciatica patients.
- Ice Application: Good for initial inflammation and muscle spasms that occur with lumbar herniated discs. This will also help with muscle spasms associated with sciatica.
- Heat Therapy: After the first 48 hours, heat may also help reduce muscle spasms that occur with both conditions.
- Physical Therapy: Certain stretching exercises are great for treating both conditions. Your doctor will be able to give you information pertaining to your specific needs.
- Epidural Injections: In cases where normal medications are not enough, your doctor may recommend steroid injections. The effects of this treatment, however, vary.
Surgical Treatment
Two minimally invasive procedures are typically used for sciatica and lumbar herniated discs. Most commonly, this includes a microdiscectomy or an endoscopic microdiscectomy. These procedures relieve the pressure on the nerve root and allow for a better healing environment.
Typically, the doctor removes only a small portion of the disc that is pressing against the nerve. The majority of the disc is left alone, structurally speaking. The doctor will use small incisions in a microdiscectomy.
For an endoscopic microdiscectomy, the doctor also uses endoscopic guidance. That really is the main difference. The doctor inserts the implements through a tiny tube to minimize damage to surrounding tissues. A small camera is also inserted through the tube to allow guidance for the performing surgeon.
Both surgeries are minimally invasive and performed on an outpatient basis.
If you are experiencing symptoms of either lumbar disc herniation or sciatica, please contact our spine doctors at (855) 853-6542. Our team is passionate about finding an individualized care plan that will work for you. Contact us today!