Spinal stenosis is not the result of a single injury. It develops gradually as the structures within the spine change over time. Discs begin to lose height. Joints thicken. Ligaments become less flexible. In some…
If you’re experiencing pain in the hips, lower back, buttocks, or legs, it could be due to an issue with the sacroiliac joint. This sometimes overlooked joint may be responsible for up to 30 percent of lower back pain.
Use this guide to understand the sacroiliac joint and how it causes your pain. Then explore some of the common treatments proven to provide relief.
What is the Sacroiliac Joint?
The sacroiliac (SI) joints connect each hip bone to the sacrum—a triangular bone at the bottom of the spine. A network of ligaments and muscles stabilizes this area. This joint has some mobility, but not very much when compared to other joints.
The SI joint supports the weight of the upper body. It transfers this weight and absorbs shock between the upper body and legs. In addition, it limits the stress between the lower spine and hip during weight-bearing activities.
Common Causes of Sacroiliac Joint Pain
As we age, the SI joint begins to change. Walking and other activities cause these once-flat joints to develop angles and curves. Pregnancy and injury can play a role in changing these joints. Structural changes can lead to spondyloarthropathy—a class of diseases that affect the joints of the vertebral column—as well as other joint issues.
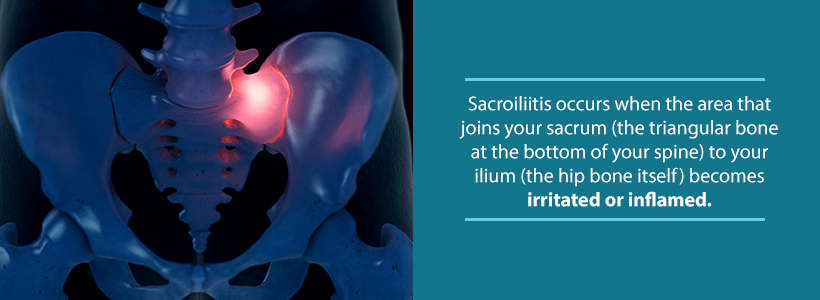
Sacroiliitis
Sacroiliitis occurs when an SI joint becomes irritated and inflamed. Several factors can cause this condition. During pregnancy, for example, the SI joints stretch and loosen to prepare for childbirth. This change, along with the added weight from carrying a child, puts extra stress on the joint leading to inflammation.
In addition, different forms of arthritis such as osteoarthritis and ankylosing spondylitis can inflame the joints. A fall or car accident may also damage the joints leading to sacroiliitis.
Symptoms of sacroiliitis include pain in the buttocks or lower back. Pain can also affect the groin, legs, and feet. This is especially true when running, climbing stairs, or bearing weight unevenly in the legs. In addition, pain and stiffness usually occur when sitting for a long time or after getting out of bed in the morning.
Sacroiliac Joint Dysfunction
This condition involves too much or little motion in the SI joint. These abnormal hip movements affect the way in which the SI joint works.
Risk factors for sacroiliac joint dysfunction include aging, pregnancy, previous lower back surgeries, and contact sports. Even simply walking can cause dysfunction if your gait puts uneven pressure on your pelvis.
Symptoms are similar to sacroiliitis, however, pain is typically felt on one side of the lower back, buttocks, or legs. In addition, you may feel instability in the pelvis and lower back. It may feel like the pelvis will “give out” when walking, standing, or rising from a chair.
Diagnosing these conditions can be tricky because the symptoms often mimic other conditions such as lumbar disc herniation or sciatica. Furthermore, there is no single test to accurately detect these conditions. To be accurately diagnosed, a doctor should discuss your medical history and conduct a complete physical exam. Diagnostic imaging like MRIs, CT scans, or X-rays also helps with diagnosing SI joint pain.
Treating Sacroiliitis and Other SI Joint Issues
Once you determine your pain involves issues with the SI joint, several treatment options are available. Here are some of the common ways to treat sacroiliitis:
Resting the Area
If you just started feeling sacroiliac joint pain, try resting the area. Taking a day or two away from normal activities can help to reduce minor symptoms. Resting the area too long, however, may cause additional stiffness and weakening of the joint.
Applying ice or heat to the affected areas can help with muscle tension and pain. Consider icing your lower back and pelvis. Then, slowly introduce heat to the area around the joint.
Pain Medication
Over-the-counter medications like acetaminophen or ibuprofen can help mild to moderate joint pain. If you’re experiencing a sudden burst of severe pain, a doctor may prescribe muscle relaxers or narcotic painkillers.
As with any prescribed medications, research the risks and benefits. Some of these drugs can have unpleasant side effects or lead to dependence. Make sure you talk to your doctor about any concerns you may have.
Sacroiliac Joint Injections
When oral medications don’t provide relief, sacroiliac joint injections can reduce pain by delivering medication directly to the source. A combination of a local anesthetic and anti-inflammatory medication can provide a period of pain relief. This will help you receive other treatments or get back to your daily activities.
TNF Inhibitors
If your joint pain is caused by an inflammatory condition such as ankylosing spondylitis or rheumatoid arthritis, your body may have high levels of Tumor Necrosis Factor (TNF). Healthy individuals block this substance naturally. Those with inflammatory conditions have higher levels of TNF in the blood.
TNF inhibitors can reduce inflammation and slow disease progression. They are usually given by injection or IV treatment. Sometimes medications are administered by professionals, but you may also be able to do it on your own.
While some patients notice a change in two or three doses, others may take up to three months to feel the drug take effect.
TNF inhibitors increase the risk of infection from tuberculosis and fungus. Those with conditions like multiple sclerosis or heart failure should not use them.
Physical Therapy
A physical therapist evaluates your condition and provides an individualized treatment program based on your needs. Physical therapists can also give insights into how your daily routines are affecting your sacroiliac joint. They also offer ideas for adaptations to prevent further irritation to the area.
Treatment from a physical therapist usually involves manual therapy to help with soft tissue tension, pelvic alignment, and joint mobilization. You also learn how to strengthen and improve flexibility in the area with targeted routines, including hip flexion exercises.
In some cases, a physical therapist may recommend wearing a sacroiliac belt to provide support and stability to your joints.
Electrical Stimulation
When pain medications and physical therapy don’t provide the relief you need, more aggressive approaches may be necessary. One common procedure involves implanting an electrical device into the sacrum. This device blocks the nerves from sending pain signals to the brain by using electrical pulses.
Radiofrequency Ablation
This minimally invasive procedure uses radiofrequency waves to heat a small needle which burns the nerve. The heat lesion disrupts the nerve’s ability to send pain signals to the brain.
Using a small incision, the doctor guides a tiny needle into the affected nerve. With the guidance of a live X-ray, the surgeon finds the targeted nerve and numbs it. Radiofrequency waves heat the tip of a needle to create a lesion. The procedure generally takes about an hour.
Pain relief usually occurs in two or three weeks. Eventually, the nerve starts to grow back, which may or may not cause the pain to return. For most successful radiofrequency ablation procedures, pain relief can last about a year.
SI Joint Fusion
In some of the most severe cases, surgery may be the best option. If non-surgical treatments haven’t helped with your pain and daily functioning, SI joint fusion may be the next option. This elective surgery is usually recommended after 2 or 3 months of trying non-surgical treatments.
Advances in medical technology have made an SI joint fusion a minimally invasive procedure. Using a small incision, usually on the side of the buttock, the surgeon inserts a bone graft into the joint and secures it with screws and pins. This allows the sacrum and hip bone to fuse together, thus decreasing excess motion.
The procedure usually takes about an hour. You may return home the same day. Since it takes time for the bones to fuse together, recovery time can be up to six months. During the recovery process, a physical therapist will work with you to restore strength and flexibility in the area.
Getting the Help You Need
If you’re experiencing pain due to SI joint issues, you want to get help from an expert orthopedic team who is familiar with this condition. Orthopedic & Laser Spine Surgery will help pinpoint your source of pain and find the most appropriate treatments based on your unique situation.
Orthopedic & Laser Spine Surgery specializes in minimally invasive techniques designed to reduce complications and speed up recovery time. Our comprehensive program uses the latest research and technology for both non-surgical and minimally invasive procedures. We want to help you return to the life you desire, so schedule an appointment today!